WHAT IS HYPOSPADIAS?
Penis birth defects such as hypospadias are among the most common birth defects in the world, more common than cleft lip/palate, Down's syndrome, or spina bifida, affecting more than 10,000 boys in the United States per year. Usually, the cause is not known. Abnormalities can include penile curvature (chordee), penile torsion, foreskin problems, and/or urinary channel problems.
With distal hypospadias, the urinary opening is near the head of the penis, but it can be located further down in boys with proximal hypospadias, as far as within the scrotum close to the anus. In addition to the abnormal appearance, the malpositioned urinary opening can result in difficulty aiming into the toilet with a spraying or misdirected stream. In some boys, the penis is bent downwards or sideways to an extent that sexual activity could be impaired as an adult – especially in those with more severe hypospadias and in boys with penile curvature (chordee) without hypospadias.
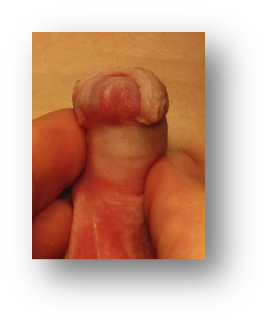
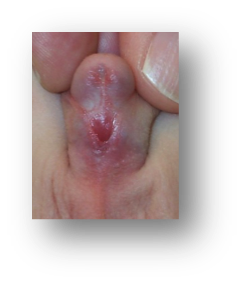
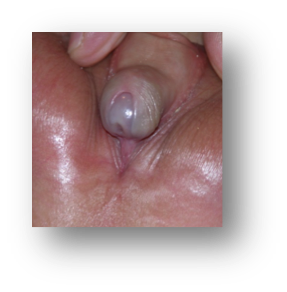
The spectrum of hypospadias, from an opening near the head of the penis (1st picture), in the middle of the penis (2nd picture), to within the scrotum (3rd picture).
Surgery is done to straighten the penis, move the urinary channel to the correct location on the head of the penis, and to either perform circumcision or to repair the partial foreskin to look complete (prepucioplasty). Different operations have been developed over the years to correct hypospadias. Today TIP is the most common operation used worldwide, better known as the “Snodgrass repair” since he described this technique in 1994.
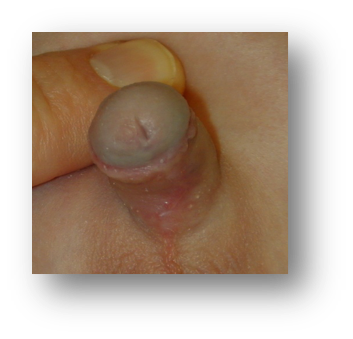
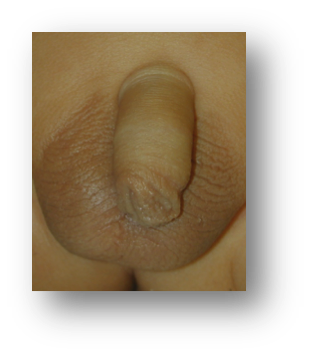
Normal appearance after TIP repair. The child on the left had circumcision, while the one on the right had the foreskin repaired (prepucioplasty).
At Hypospadias Specialty Center, we specialize in reconstruction of penile birth defects in both children and adults. For nearly 20 years, our doctors have monitored results and made improvements when needed to provide among the best functional and cosmetic outcomes. In contrast to general pediatric urologists, who operate on distal hypospadias an average of once per month (ref), our team repairs hypospadias 4-5 days per week.